Alive Inside
- IPPP

- Oct 9, 2019
- 1 min read
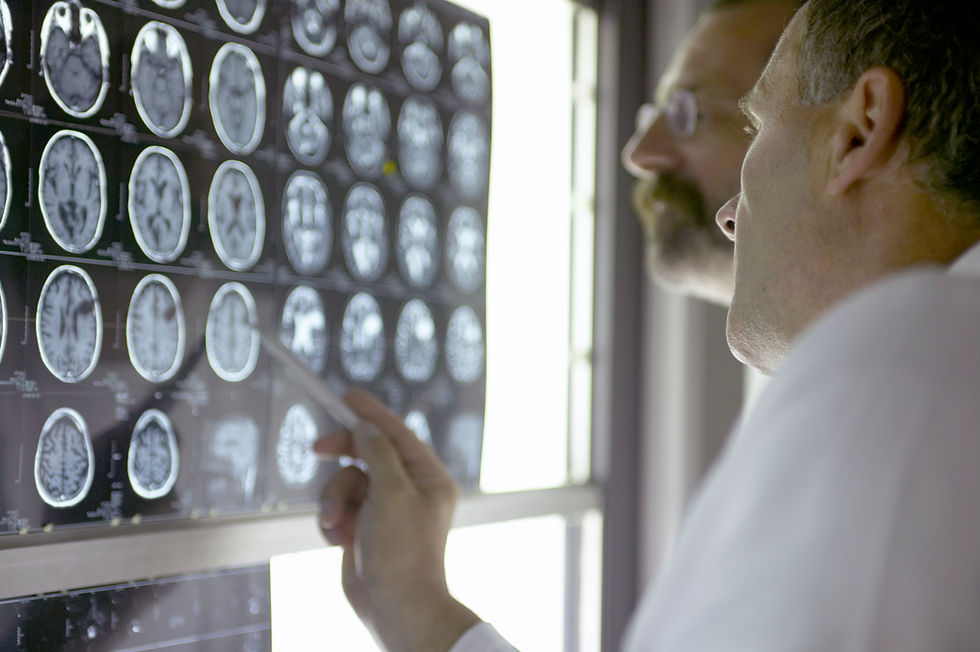
Brain scans reveal that some unresponsive brain-injured patients are actually conscious. But what should clinicians do with this information?
Andrew Peterson (IPPP, George Mason University), Adrian M. Owen (Brain and Mind Institute, University of Western Ontario), and Jason Karlawish (Penn Memory Center, University of Pennsylvania) publish new commentary on the U.S. Practice Guideline Update on Disorders of Consciousness: https://onlinelibrary.wiley.com/doi/full/10.1111/bioe.12678
Key takeaway #1: The recent U.S. practice guideline update on DoC is a milestone in the history of neurology, as it recommends the use of investigational neuroimaging methods to assess brain-injured patients.
Key takeaway #2: The ethical issues raised by the disclosure of neuroimaging results to brain-injured patients' families are similar to those observed in other domains of medicine, where pre-clinical neuroimaging results are shared, such as Alzheimer's disease research.
Key takeaway #3: The DoC research and clinical communities need a systematic procedure for disclosing evidence of covert consciousness to patients' families.
Key takeaway #4: We need to develop methods that provide insight into the subjective quality of life of covertly conscious patients.
Key takeaway #5: We need to address the cost of neuroimaging to detect covert consciousness, and the complexity of justifying that cost without having a clear sense of how neuroimaging assessment influences the quality of life of these patients.




Comments